Peptides for weight loss side effects range from mild nausea to rare but serious complications like pancreatitis, and understanding them before starting therapy could save someone a lot of misery. With GLP-1 agonists like semaglutide and tirzepatide now mainstream, and next-generation options like retatrutide showing up to 28.7% mean weight loss in Phase 3 trials, more people than ever are considering peptide therapy for obesity. But the conversation around results often drowns out the risks.
This guide breaks down exactly what happens in the body when weight loss peptides go to work, which side effects are common versus dangerous, who faces the highest risk, and how proper medical oversight can make a real difference. Whether someone is exploring FDA-approved peptides for weight loss or watching investigational compounds move through clinical trials, they deserve a clear picture, not marketing spin, of what these therapies actually feel like day to day.
How Weight Loss Peptides Work in Your Body
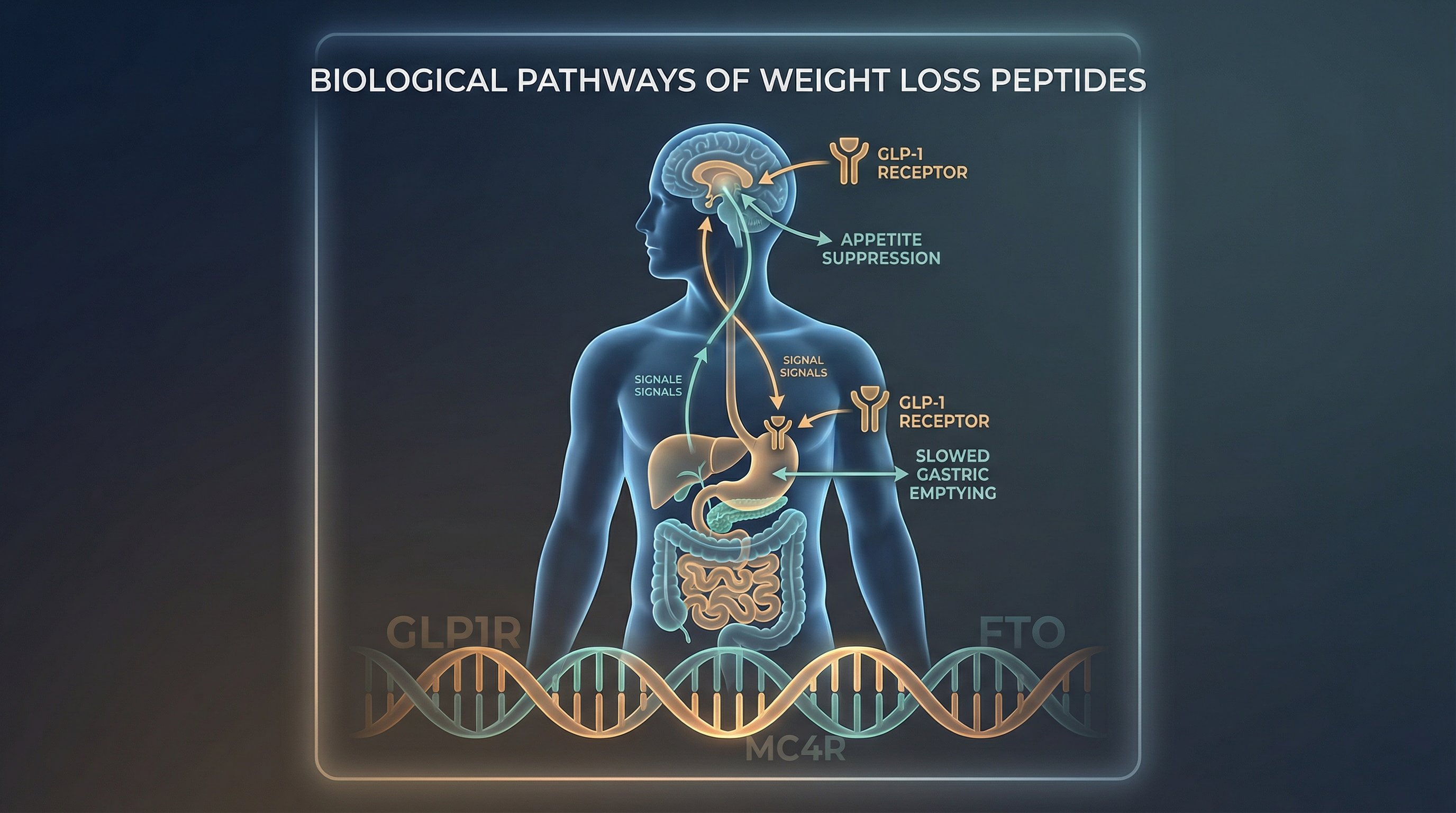
Weight loss peptides don't burn fat directly. Instead, they mimic natural hormones that regulate appetite, blood sugar, and metabolism. The most studied class, GLP-1 receptor agonists, works by binding to receptors in the gut and brain that control hunger signals.
When someone injects semaglutide or tirzepatide, the peptide activates GLP-1 receptors in the hypothalamus. This triggers a feeling of fullness and reduces food cravings. At the same time, these peptides slow gastric emptying, meaning food stays in the stomach longer. That's why many patients report feeling satisfied with smaller meals.
But the mechanism goes deeper than appetite suppression:
- GLP-1 agonists (semaglutide, liraglutide) enhance insulin sensitivity and improve glucose regulation
- Dual agonists like tirzepatide activate both GLP-1 and GIP receptors, producing stronger metabolic effects
- Triple agonists like retatrutide target GLP-1, GIP, and glucagon receptors simultaneously, adding a hepatic fat metabolism component
- Growth hormone secretagogues (ipamorelin, sermorelin) stimulate natural GH release, which supports fat breakdown and lean mass preservation
Each mechanism carries its own side effect profile. GLP-1 agonists primarily affect the gastrointestinal system. Growth hormone peptides tend to impact glucose metabolism and fluid balance. Understanding which pathway a peptide targets helps predict which side effects to expect. For those specifically targeting abdominal fat, our guide on peptides for belly fat covers which options are most effective.
Genetic variation also plays a significant role. Variants in genes like GLP1R, MC4R, FTO, and TCF7L2 can affect how strongly someone responds to a given peptide, and how severe their side effects are. According to pharmacogenomic research, genetic differences create a 30% to 70% variance in individual response to peptide therapy. Two people on the same dose of the same peptide can have completely different experiences.
Common Side Effects of Weight Loss Peptides
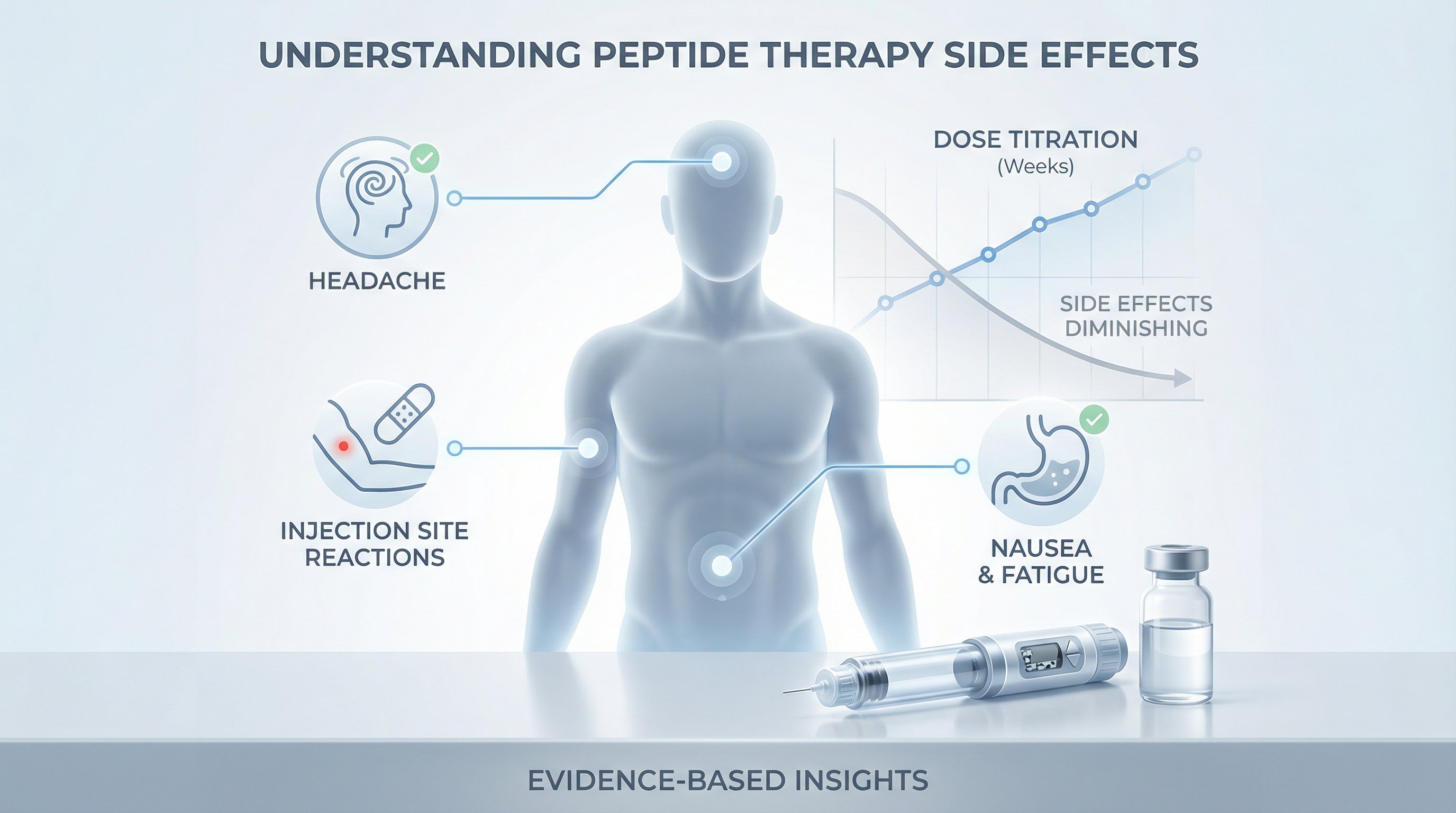
The most frequently reported peptides for weight loss side effects are gastrointestinal. This isn't surprising, these drugs work by altering gut motility and appetite signaling. The GI tract takes the brunt of it, especially during the first weeks of treatment.
Clinical trial data for semaglutide shows the following incidence rates for common side effects:
- Nausea: 44% of patients
- Diarrhea: 30%
- Vomiting: 24%
- Constipation: 24%
- Decreased appetite (which is technically the intended effect, but can feel unpleasant)
Tirzepatide numbers are slightly different but follow the same pattern, nausea at roughly 33%, diarrhea at 23%, and constipation at up to 25%.
Beyond GI symptoms, patients commonly report:
- Injection site reactions, redness, swelling, or mild pain at the injection area
- Headaches, particularly during the first two weeks
- Fatigue and dizziness, usually transient and dose-related
Here's the good news: most common side effects decrease over time. The standard clinical approach is to start at a low dose and titrate upward slowly. The standard semaglutide dose chart, for instance, begins at 0.25 mg weekly and increases over 16–20 weeks to the target dose. Patients who escalate too quickly almost always experience worse GI symptoms.
Growth hormone peptides like ipamorelin and sermorelin have a different common side effect profile. Facial flushing, mild headache, and injection site reactions are typical. MK-677 (an oral GH secretagogue) can cause increased appetite, which is counterproductive for weight loss, along with water retention and muscle pain.
The pattern is consistent across peptide classes: side effects are usually worst during initiation and dose changes, then settle down within a few weeks.
Serious and Rare Side Effects to Watch For
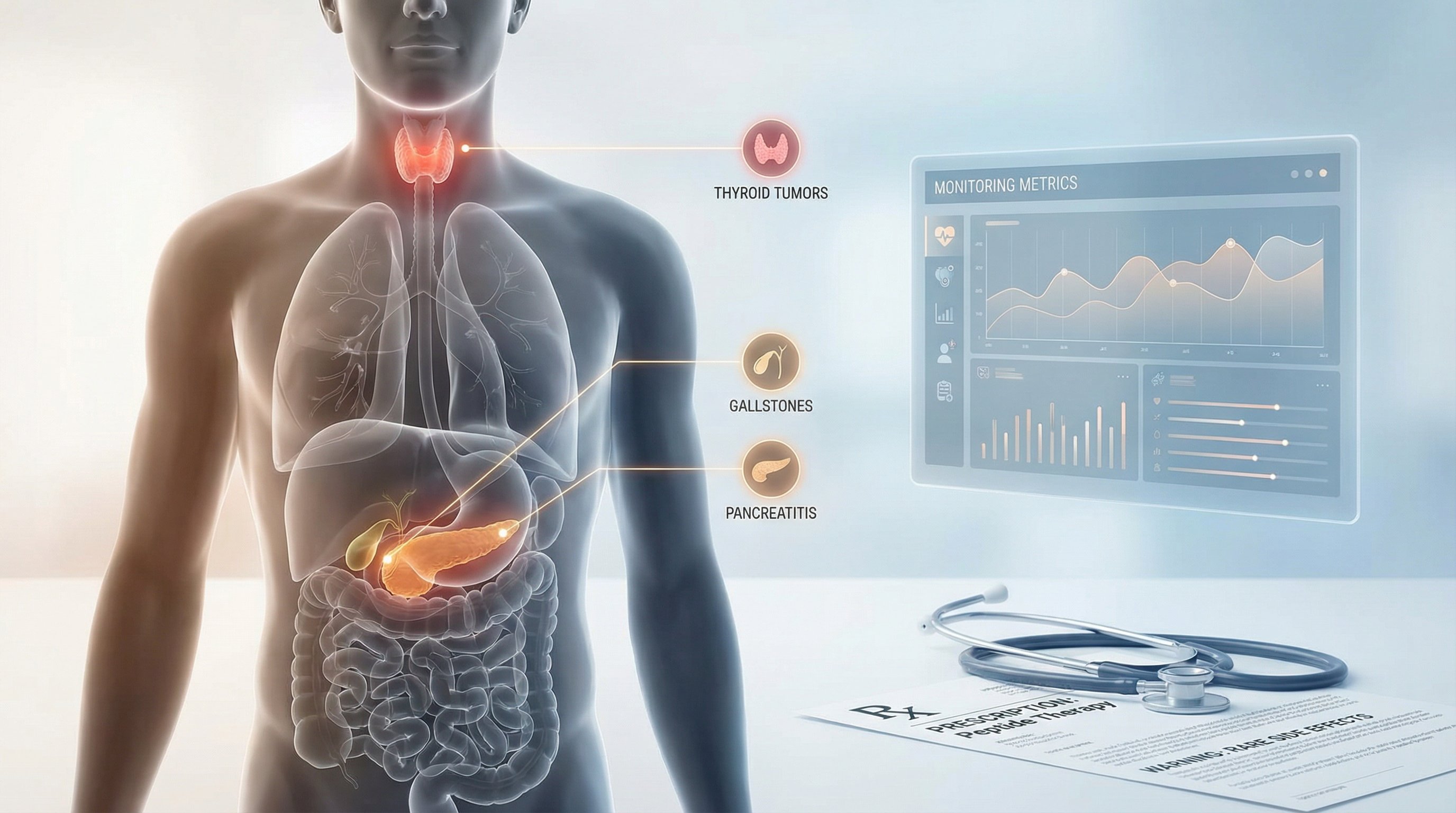
While most people tolerate weight loss peptides reasonably well, some side effects are genuinely dangerous. These are rare, but anyone considering peptide therapy needs to know they exist.
Pancreatitis
Both semaglutide and tirzepatide carry a pancreatitis warning in their prescribing information. Symptoms include severe abdominal pain radiating to the back, nausea, and vomiting that doesn't improve. Baseline amylase and lipase blood tests are recommended before starting therapy. If pancreatitis develops, the peptide must be discontinued immediately.
Gallbladder Events
Rapid weight loss from any cause increases gallstone risk. GLP-1 agonists compound this by altering gallbladder motility. Patients losing weight quickly on these peptides should be monitored for gallbladder symptoms, sharp right-sided abdominal pain, especially after eating fatty foods.
Medullary Thyroid Carcinoma (MTC) Risk
Semaglutide, tirzepatide, and liraglutide all carry a boxed warning about medullary thyroid carcinoma. This comes from animal studies showing thyroid C-cell tumors in rodents. The relevance to humans isn't fully established, but anyone with a personal or family history of MTC or Multiple Endocrine Neoplasia type 2 (MEN2) should absolutely avoid these peptides.
Other Serious Concerns
- Gastroparesis, severely delayed stomach emptying that goes beyond the intended therapeutic effect
- Hypoglycemia, particularly when peptides are combined with insulin or sulfonylureas
- Vision changes, reported in some diabetic patients on semaglutide, possibly related to rapid blood sugar improvement
- Allergic reactions, rare but documented anaphylaxis cases exist
For investigational peptides like retatrutide, the full safety profile is still being established. Phase 3 trials are expected to report data in 2026, but long-term side effects beyond 68 weeks remain unknown.
Unapproved peptides purchased from unregulated sources carry additional risks, including contamination, incorrect dosing, and unknown degradation products. This is not a theoretical concern, it's a documented problem in the peptide marketplace.
Who Is Most at Risk for Peptide Side Effects

Not everyone faces equal risk when starting weight loss peptide therapy. Certain medical histories, genetic factors, and lifestyle variables significantly increase the chance of adverse reactions.
People who should exercise extra caution, or avoid specific peptides entirely:
- History of medullary thyroid carcinoma or MEN2, GLP-1 agonists are contraindicated
- History of pancreatitis, GLP-1 and dual agonists increase recurrence risk
- Severe gastroparesis or GI conditions, peptides that slow gastric emptying can worsen symptoms dramatically
- Type 1 diabetes or insulin-dependent patients, hypoglycemia risk increases substantially
- Pregnancy or breastfeeding, no adequate safety data exists for any weight loss peptide
- Eating disorders, powerful appetite suppression can worsen disordered eating patterns
Genetic factors matter too. People with certain GLP1R receptor variants may experience stronger GI side effects at standard doses. Those with FTO gene variants associated with higher baseline BMI may need different titration schedules. And TCF7L2 variants can alter glycemic response, affecting both efficacy and hypoglycemia risk.
Age and metabolic health also play a role. MK-677, for example, showed a 6.5% congestive heart failure rate in an elderly trial population, a serious safety signal that led to development being discontinued for that indication. Younger, metabolically healthy individuals tolerate it much better.
People taking multiple medications face additional risk from drug interactions. Weight loss peptides can alter the absorption rate of oral medications because they change how quickly food and drugs move through the stomach. Anyone on time-sensitive medications, like oral contraceptives, thyroid hormones, or blood thinners, needs their physician to review timing and dosing.
The bottom line on risk: the more complex someone's health profile, the more critical proper medical supervision becomes.
How to Minimize Side Effects With Proper Medical Supervision

The single most effective strategy for reducing peptides for weight loss side effects is working with a qualified provider who understands dose titration, monitoring protocols, and individual risk factors.
Start Low, Titrate Slow
This phrase gets repeated constantly in peptide therapy for good reason. Clinical trials consistently show that patients who escalate doses too quickly experience significantly worse GI symptoms. The standard semaglutide protocol starts at 0.25 mg weekly and increases every four weeks. Tirzepatide follows a similar step-wise approach starting at 2.5 mg weekly. Skipping steps or accelerating the schedule is the most common cause of intolerable side effects.
Baseline and Ongoing Bloodwork
Proper monitoring catches problems before they become dangerous. A responsible provider will order:
- Lipid panel, baseline and at 12 weeks
- Thyroid function (TSH, fT4), baseline, especially given the MTC boxed warning
- Amylase and lipase, baseline pancreatitis screening
- Comprehensive metabolic panel, baseline and at 12 weeks to check liver and kidney function
- Fasting glucose and HbA1c, to track metabolic changes
Source Quality Matters
FDA-approved peptides obtained through licensed pharmacies have verified potency, purity, and sterility. Compounded peptides from 503A or 503B pharmacies are legal with a prescription but vary in quality. Research-grade peptides purchased online carry the highest contamination risk.
Report Symptoms Early
Many patients try to power through side effects, assuming they'll pass. Some will. But persistent vomiting, severe abdominal pain, or unusual swelling need prompt medical attention. Catching pancreatitis or gallbladder events early dramatically changes outcomes.
Platforms like Peptide Injections can help patients connect with board-certified physicians who specialize in peptide therapy, taking the guesswork out of finding a qualified provider who understands proper titration, monitoring, and risk management.
Lifestyle Adjustments That Help
- Eat smaller, more frequent meals to reduce nausea
- Stay well hydrated, dehydration worsens GI symptoms
- Prioritize protein intake to prevent lean mass loss during weight reduction
- Avoid high-fat meals, which compound delayed gastric emptying discomfort
How to Decide if Peptide Therapy Is Right for You
Peptide therapy for weight loss isn't for everyone, and it shouldn't be a first-line approach for someone who's mildly overweight and hasn't tried lifestyle changes. The strongest evidence supports use in specific populations.
FDA-approved GLP-1 agonists are indicated for:
- BMI ≥30 (obesity)
- BMI ≥27 with at least one weight-related comorbidity (type 2 diabetes, hypertension, dyslipidemia)
Beyond the clinical criteria, there are practical questions worth asking:
- Has the person genuinely tried dietary and exercise interventions? Peptides work best as an addition to lifestyle changes, not a replacement.
- Can they commit to ongoing medical monitoring? Blood work, follow-up appointments, and dose adjustments aren't optional, they're essential for safety.
- Are they comfortable with injections? Most weight loss peptides require subcutaneous injections, either daily or weekly.
- Do they understand this may be long-term therapy? Weight regain after stopping GLP-1 agonists is well-documented. Some patients need indefinite treatment to maintain results.
- Is cost sustainable? Branded semaglutide and tirzepatide remain expensive, and insurance coverage varies widely.
For people with severe obesity (BMI ≥40) who've had partial response to single-agent GLP-1 therapy, investigational options like retatrutide or CagriSema may be worth discussing with a provider, though these remain available only through clinical trials as of early 2026.
Anyone considering peptide therapy should start with an honest conversation with a physician who specializes in metabolic health. Not a wellness influencer. Not a Telegram group. A qualified medical professional who can evaluate their full health picture, order appropriate genetic and metabolic testing, and build a protocol matched to their biology.
Peptide Injections offers an AI-powered matching system that connects patients with specialized peptide therapy providers in about two minutes, making it easier to find a board-certified physician without hours of independent research.
Conclusion
Peptides for weight loss side effects are real, predictable, and, in most cases, manageable with proper medical guidance. The GI symptoms that dominate early treatment typically improve with slow dose titration. Serious risks like pancreatitis and thyroid concerns, while rare, demand baseline screening and ongoing monitoring.
The key takeaway? Side effects aren't a reason to avoid peptide therapy. They're a reason to approach it correctly. That means working with a knowledgeable provider, getting bloodwork done on schedule, using verified pharmaceutical sources, and reporting symptoms promptly.
Weight loss peptides represent some of the most effective tools available for treating obesity in 2026. But effective tools still require skilled hands. Anyone serious about this path should start with a medical professional who treats peptide therapy as the clinical intervention it is, not a shortcut.
Frequently Asked Questions About Peptides for Weight Loss Side Effects
What are the most common peptides for weight loss side effects?
The most common side effects are gastrointestinal: nausea (44% with semaglutide), diarrhea (30%), vomiting (24%), and constipation (24%). Injection site reactions, headaches, and fatigue also occur frequently but typically improve within weeks with slow dose titration.
How do weight loss peptides work in the body?
Weight loss peptides mimic natural hormones to regulate appetite, blood sugar, and metabolism. GLP-1 agonists bind to receptors in the gut and brain to create fullness signals and slow gastric emptying. Dual agonists like tirzepatide activate multiple receptors for stronger effects.
Are there serious side effects from peptides for weight loss I should know about?
Yes. Rare but serious risks include pancreatitis, gallbladder events, gastroparesis, and hypoglycemia. GLP-1 agonists carry a medullary thyroid carcinoma boxed warning from animal studies. Baseline blood work for amylase, lipase, and thyroid function helps screen for these risks before starting therapy.
Who should avoid or use caution with weight loss peptides?
People with a history of medullary thyroid carcinoma, MEN2, pancreatitis, severe gastroparesis, type 1 diabetes, pregnancy, or eating disorders should avoid or exercise extreme caution. Those on multiple medications or with complex health profiles need careful physician oversight to manage interactions and individual risk factors.
How can I minimize side effects when using peptides for weight loss?
Start with low doses and titrate slowly—semaglutide typically starts at 0.25 mg weekly, increasing every four weeks. Obtain baseline and ongoing bloodwork (lipid panel, thyroid, amylase/lipase). Use FDA-approved peptides from licensed pharmacies, eat smaller meals, stay hydrated, and report symptoms promptly to your provider.
Do genetic factors affect how I'll respond to peptides for weight loss?
Yes. Variants in genes like GLP1R, MC4R, FTO, and TCF7L2 create 30–70% variance in individual response to peptide therapy. Genetic differences influence how strongly someone responds, the severity of side effects, and glycemic response. Pharmacogenomic testing can help identify your optimal protocol.